Dental implantology is an advanced dental solution that allows you to replace one or more missing teeth through the placement of dental implants. The loss of a tooth affects more than just the aesthetics of your smile: it can affect your chewing, alter the balance of your jaw, promote the shifting of neighboring teeth, and impact your quality of life.
For this reason, dental implantology must be considered a personalized clinical approach, aimed at restoring stable chewing function and a natural aesthetic result to the patient. In this scenario, the quality of the devices and components used in the production of dental implants plays a key role in the precision, reliability, and safety of the treatment.
The goal is not simply to replace a missing tooth, but to reconstruct a condition as close to the natural one as possible, both functionally and aesthetically. A proper evaluation of dental implantology therefore requires considering several factors: clinical indications, materials used, procedure, healing time, expected implant lifespan, and the economic sustainability of the treatment.
What is dental implantology?
Dental implantology, or implant dentistry, is the branch of dentistry that deals with replacing missing teeth using implants inserted into the maxillary or mandibular bone. Implants act as artificial roots and are used to support crowns, bridges, or dentures.
Depending on the clinical situation, an implant can replace a single tooth, multiple adjacent teeth, or entire dental arches. If a single tooth is missing, treatment generally involves the placement of an implant and the application of a crown. When multiple teeth are missing, rehabilitation may require multiple implants and a more complex prosthetic solution.
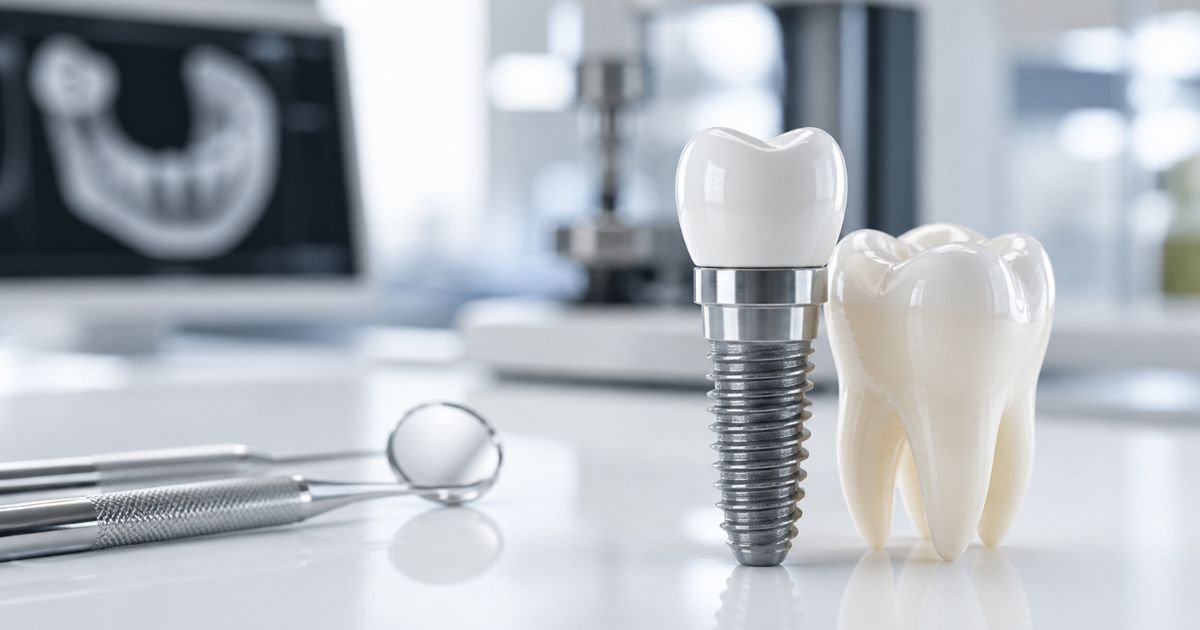
A dental implant is normally composed of three main elements:
- the implant screw, inserted into the bone;
- the abutment, which connects the implant and the prosthesis;
- the crown, bridge or prosthesis, that is, the visible part of the rehabilitation.
This structure allows for a stable, durable result that resembles a natural tooth. The value of dental implants is therefore not limited to aesthetic tooth replacement, but rather involves restoring the entire balance of the mouth.
Why tooth loss should not be underestimated
The loss of one or more teeth can be caused by a variety of factors: deep decay, periodontitis, trauma, fractures, infections, or progressive weakening of the supporting tissues. Whatever the origin of the problem, a gap left within the arch can have long-term consequences.
Neighboring teeth can tilt, those in the opposing arch can shift into the free space, and chewing can become less balanced. Furthermore, when the tooth’s natural root is missing, the bone no longer receives the functional stimuli for chewing and can undergo resorption.
This aspect is particularly important because bone quantity and quality are decisive factors in evaluating the possibility of placing an implant. Waiting too long after tooth loss can make subsequent implant rehabilitation more difficult.
What is dental implantology for?
Dental implants are used to replace missing teeth and restore stable chewing function. Depending on the case, they can be used to treat a single tooth, multiple teeth, or an entire arch.
The main implant solutions include:
- single crown on implant, indicated when only one tooth is missing;
- bridge on implants, indicated when several adjacent teeth are missing;
- fixed prosthesis on implants, for more extensive rehabilitations;
- removable prosthesis stabilized by implants, useful in some cases of partial or total edentulism.
The choice depends on several factors: the number of missing teeth, bone condition, gum health, aesthetic expectations, functional needs, the patient’s age, oral hygiene habits, and general clinical picture.
Who can undergo dental implant treatment?
Not all patients have the same access to dental implants. Before proceeding, the dentist must assess whether the clinical conditions exist for safe and predictable implant placement.
One of the main criteria is the presence of a sufficient amount of bone. The implant must be supported by adequate bone tissue, capable of ensuring its initial stability and subsequent integration. If there is insufficient bone, the treatment plan may include preliminary procedures such as bone regeneration, grafts, or sinus lift.
Gum health is also crucial. Uncontrolled periodontitis, active infections, or poor oral hygiene can increase the risk of complications. For this reason, before surgery, your dentist may recommend preparatory treatments to stabilize your oral health.
The patient’s general condition must also be evaluated. Uncontrolled diabetes, specific drug therapies, heavy smoking, systemic diseases, or conditions that reduce healing capacity may require greater caution. This does not mean that implantology is always ruled out, but rather that the approach must be personalized.
The role of the dentist in implant evaluation
Choosing a dentist is one of the most important aspects of the entire process. Implantology requires surgical, prosthetic, diagnostic, and design expertise. The dentist must not simply place an implant, but must evaluate the patient’s entire mouth: tooth position, occlusion, bone quality, smile aesthetics, and future maintenance of the rehabilitation.
The dental instruments used in the various clinical phases also contribute to operational precision and correct treatment management.
A thorough implantology consultation includes a medical history, clinical examination, radiographic evaluation, possible 3D CT scan, gum analysis, and the development of a treatment plan. Only after this phase can we determine whether dental implantology is truly the most suitable solution.
Dental implant materials: titanium and zirconia
The most widely used material in dental implantology is titanium. It is prized for its biocompatibility, mechanical strength, and ability to integrate with bone through the process of osseointegration. For this reason, titanium remains the gold standard in most implant treatments. In the dental field, Oros processes titanium to create precision components such as dental implants, abutments, prosthetic screws, and implant elements, using CNC bar processes designed for stability, repeatability, and dimensional control.
In some cases, zirconia implants may also be considered. Zirconia is a white ceramic material, sometimes used for aesthetic reasons, especially in the anterior region, or in patients who prefer metal-free solutions. It may also be considered in patients with particular sensitivities, always after a specialist evaluation.
The choice between titanium and zirconia depends on more than just color or patient preference. The dentist must consider implant position, masticatory loads, bone quality, prosthetic type, gum health, and aesthetic goals. In implantology, the most suitable material is the one consistent with the specific clinical case.
How does implant treatment work?
Implant treatment is not a single, isolated procedure, but a multi-stage process. The first is diagnostic: the dentist assesses the patient’s mouth, gathers information about their general health, analyzes X-rays, and determines whether there is sufficient bone.
The second phase is planning. It determines where to place the implants, how many implants to use, and what type of prosthesis to create. This is followed by the surgical phase, during which the implants are positioned in the bone.
After the surgery, the healing and osseointegration phase begins. Finally, once the implants are stable, the definitive prosthesis is applied.
Dental implant techniques
Modern implantology uses increasingly precise techniques, designed to make treatment safer, more predictable, and, where possible, less invasive.
Guided computer planning
Computer-guided planning allows you to plan the implant position before surgery. Through three-dimensional examinations and dedicated software, the dentist can assess bone volume, nerve position, distance from the maxillary sinus, and the most appropriate implant inclination.
This technology allows treatment to be designed based on the future prosthesis, improving the precision of implant placement. In some cases, digital planning also allows the use of customized surgical guides.
Immediate loading implantology
L’implantologia a carico immediato permette, in casi selezionati, di applicare una protesi provvisoria sugli impianti entro tempi molto brevi dall’intervento. Questa soluzione può offrire un vantaggio estetico e funzionale importante, perché il paziente non rimane senza denti durante la fase di guarigione.
Immediate loading, however, isn’t suitable for everyone. To perform it safely, specific conditions are required: good primary stability of the implants, adequate bone, proper load distribution, and careful prosthetic design.
Traditional implantology
In traditional implantology, after implant placement, a period of osseointegration is allowed before the final prosthesis is applied. This technique is widely used and allows for the biological time required for the implant to stabilize in the bone.
It is a particularly suitable solution when the case requires caution, when the quality of the bone does not allow immediate loading or when regenerative procedures have been performed.
Dental implant surgery: what to expect
Dental implant surgery is generally performed under local anesthesia. In some cases, especially in anxious patients or for more complex treatments, conscious sedation may be considered.
The process usually includes the following phases:
- preliminary visit and anamnesis;
- radiographic examinations and bone assessment;
- treatment planning;
- surgical insertion of implants;
- healing period;
- periodic checks;
- application of the temporary or definitive prosthesis;
- maintenance program.
The duration of the procedure depends on the number of implants, their position, anatomical complexity, and any need for additional treatments. A single implant may require relatively little time, while a complete rehabilitation requires more detailed planning.
Healing times and osseointegration
After the implant is inserted, the body begins the process of osseointegration. The bone gradually bonds to the implant surface, creating a stable base for the future prosthesis.
In many cases, integration times range from 3 to 6 months, but may vary depending on the area treated, bone quality, patient health, and the technique used. In cases of immediate loading, the patient can receive a temporary prosthesis quickly, but this does not eliminate the need to respect biological healing.
During this period, it is essential to follow the dentist’s instructions, attend check-ups, and maintain careful oral hygiene.
Post-operative care after dental implants
Postoperative care is a crucial phase of treatment. After surgery, the patient must follow the instructions received to promote healing and reduce the risk of complications.
During the first few hours, it’s important to avoid touching the treated area, rinsing your mouth vigorously, eating very hot foods, and avoiding strenuous physical activity. Your dentist may prescribe medications, mouthwashes, or specific therapies based on your specific needs.
In the first few days, it’s best to eat soft, warm foods, avoiding hard, crunchy, spicy, or very hot foods. Smoking should also be avoided, as it can slow healing and increase the risk of implant failure.
Oral hygiene must be thorough but gentle. The mouth must remain clean, but the surgical area must not be traumatized. Post-operative check-ups allow the dentist to monitor the healing process and intervene promptly if necessary.
Risks and possible complications
Dental implantology is a safe and well-established procedure, but like any surgical procedure, it can carry some risks. Possible complications include infection, bleeding, swelling, post-operative pain, damage to nearby anatomical structures, or failure of the implant to osseointegrate.
Another risk to consider is peri-implantitis, an inflammation of the tissues around the implant that, if left untreated, can compromise the stability of the restoration. Prevention involves proper oral hygiene, regular checkups, and professional maintenance sessions.
The likelihood of complications is reduced when the case is carefully studied, when the patient is suitable for treatment, and when the instructions received before and after the procedure are followed.
How long do dental implants last?
Dental implants can last for many years and, under favorable conditions, even decades. However, their lifespan is not the same for all patients and depends on numerous factors.
Among the elements that influence the longevity of the implants are:
- bone quality and quantity;
- correct surgical planning;
- precision of the prosthesis;
- daily oral hygiene;
- periodic checks;
- smoke;
- bruxism;
- gum disease;
- general health conditions.
It’s important to distinguish between an implant and a denture. An implant inserted into the bone can last a long time, while a crown or denture may require maintenance, repair, or replacement over time due to wear and tear or changes in the mouth.
For this reason, dental implantology doesn’t end with the placement of the permanent tooth. Maintenance is an integral part of long-term success.
Dental implantology and oral hygiene
Implants can’t decay like natural teeth, but the tissues surrounding them can become inflamed. For this reason, oral hygiene is essential even after implant rehabilitation.
Patients must properly use a toothbrush, interdental instruments, and, if recommended, specific devices to clean around implants. Regular professional hygiene sessions allow for gum health checks, denture stability, and the presence of any inflammation.
Good daily maintenance helps protect the investment made and preserve the results obtained with implantology over time.
Cost of dental implants
The cost of dental implants can vary greatly from case to case. There is no single price, as each treatment depends on clinical, technical, and prosthetic factors.
Factors that affect cost include:
- number of systems to be inserted;
- type of prosthesis to be made;
- materials used;
- possible need for bone regeneration;
- diagnostic tests;
- surgical complexity;
- checks and maintenance.
A single tooth replacement costs a different amount than a complete rehabilitation. Likewise, a simple case is different from a treatment requiring bone grafts, immediate loading, or advanced digital design.
To accurately assess the price, it is always advisable to request a detailed quote, indicating the phases included and any additional services.
Insurance, coverage and payment options
Dental implants are often performed privately. However, some health insurance plans, supplemental funds, or corporate welfare plans may provide full or partial reimbursement for dental and implant services.
Coverage depends on your insurance policy, maximum coverage, deductibles, exclusions, and required documentation. Before starting treatment, it’s a good idea to check whether your health plan covers dental implants or certain phases of the process.
Many dental practices also offer installment payment options or dedicated financing. Before choosing a payment option, it’s important to evaluate terms, term, potential interest, and additional costs.
Advantages of dental implantology
Dental implantology offers numerous advantages over other rehabilitation solutions, especially when the case is planned correctly.
The main benefits are:
- recovery of chewing function;
- improving the aesthetics of the smile;
- greater stability than many removable prostheses;
- possibility of replacing a tooth without filing down the adjacent teeth;
- arch stability support;
- comfort in everyday life;
- natural result, if the prosthesis is well designed.
These advantages must be evaluated on an individual patient basis. There is no one-size-fits-all solution: the implant plan must be tailored to the actual clinical situation.
Come scegliere il dentista per l’implantologia
Choosing a dentist is one of the most important steps. Implantology requires diagnosis, surgical experience, prosthetic expertise, and planning skills. Good implant treatment begins with a comprehensive view of the mouth, not just the individual implant.
Before starting, it’s helpful to ask for clear explanations about the treatment plan, materials, timing, costs, alternatives, and potential risks. The patient must be able to understand the process, know what to expect, and receive precise instructions for long-term maintenance.
Relying on professionals who are experts in dentistry and implantology means increasing the chances of obtaining a stable, functional and aesthetically consistent result..
Excellence in the production of dental implants for third parties
Dental implants can be an effective solution for replacing missing teeth, restoring chewing ability, and improving your smile. However, it shouldn’t be considered a one-size-fits-all procedure: every patient has different conditions, from bone density to gum health, to aesthetic and functional expectations.
Alongside the dentist’s clinical expertise, the quality of the implant components also contributes to the precision and reliability of the treatment. In this field, Oros positions itself as a specialized partner in the contract manufacturing of dental implants and implantology components, providing expertise in precision micromechanics, CNC machining, and dimensional control to dental companies.